One thing that we all have in common is we all get sick. Sicknesses can be caused by viruses or bacteria, and treatment depends on the cause. Bacterial infections are treated with antibiotics. Antibiotics work by helping the body’s immune system kill bacteria or stop bacteria from multiplying. Medication travels through the bloodstream into the body to seek out bacterial cells. Antibiotics vary and are used to fight different types of bacteria. The two main categories of antibiotics are:
- Broad-spectrum antibiotics: These are used to treat a wide variety of bacteria.
- Narrow-spectrum antibiotics: These can treat only a few specific types of bacteria.
Different families of antibiotics kill bacteria in their own way, some work to destroy the cell walls of bacteria and others destroy the way the cell works.
Types of Antibiotics
- Beta-lactam: This group of antibiotics kills bacteria that are surrounded by a cell wall. Some bacteria links molecules to form a cell wall and beta-lactam antibiotics block this process. The bacteria membrane bursts from pressure without the cell wall. This family falls under the broad-spectrum antibiotic category.
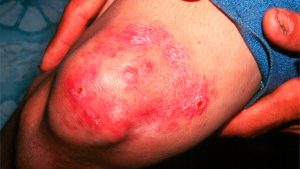
- Macrolides: These antibiotics target the ribosomes, which produce protein in human cells and bacteria. Macrolides only block bacteria from building protein. Without protein, bacteria cells cannot survive. Macrolides are commonly used to treat skin infections and respiratory tract infections.
- Quinolones: These antibiotics work by breaking down the DNA strands of bacteria. The bacteria cannot repair the DNA strands and thus cannot reproduce or survive. This group of antibiotics is used to treat infections such as bronchitis and pneumonia.
Other illnesses treated with antibiotics include:
- Strep throat.
- Whooping cough.
- Urinary tract infection.
- Sinus infection.
Antibiotics should be used to treat bacterial infections that are unlikely to clear up without treatment, are contagious, take too long to clear up or have a high risk of complications. Doctors are more likely to prescribe antibiotics to those with ongoing health conditions (asthma, diabetes, lung disease), the elderly and people with a weak immune system (for example, those with HIV).
When are Antibiotics the Wrong Treatment?
It may be tempting to reach for medication when you have a cold, flu or sore throat but these all fall under the virus category and antibiotics cannot cure these kinds of illnesses or relieve symptoms. If you are experiencing any symptoms associated with a bacterial or viral illness, go to your doctor right away to determine the exact cause. It is important to know whether you are suffering from a bacterial or viral infection as it is key to your treatment plan.
Forms of Antibiotics
Antibiotics can be administered in several different ways:
- Oral antibiotics: Tablets, capsules, liquids.
- Topical antibiotics: Creams, lotions, sprays or drops (for skin infections).
- Antibiotic injections: Drip infusions into the blood or muscle (reserved for severe infections).
Always take your full prescribed course of antibiotics even if symptoms begin to clear up.
Risks an Side Effects
Talk to your doctor before taking any antibiotic. Your healthcare professional should be fully aware of your entire health history before prescribing an antibiotic. Allergic reactions to antibiotics can cause anaphylaxis, which falls under the category of medical emergency. According to the Centers for Disease Control and Prevention (CDC):
- Antibiotics are the most common cause of emergency department visits for adverse drug events in children under 18 years old.
- Antibiotics are responsible for one in five emergency department visits for adverse drug events.
Up to 10 per cent of people who take antibiotics will experience side effects such as:
- Stomach problems.
- Diarrhea.
- Nausea.
- Vomiting.
- Thrush infections.
- Vaginal discharge, itchiness and pain.
Talk to your doctor about side effects before taking any antibiotics.
Antibiotic Resistance
A problem facing the medical community is the growing resistance of bacteria to antibiotics. These drugs have been used since the 1940s and infectious organisms have adapted and mutated over time to resist treatment. In some cases, bacteria can become resistant to antibiotics through contact with other antibiotic-resistant bacteria. According to the CDC, at least two million people in the United States will become infected with antibiotic-resistant bacteria each year and at least 23,000 people die as a result. The more often antibiotics are used, the higher the chances are for bacteria to become resistant and doctors will have fewer treatment options. The World Health Organization (WHO) has listed antibiotic resistance as one of the greatest threats to global public health. The CDC recommends the following tips to prevent antibiotic resistance:
- Talk to your doctor about steps to treat your illness without the use of antibiotics if that is an option.
- Discard old medications.
- Never skip a medication dose.
- Never take an antibiotic for a viral infection such as a cold or the flu.
- Never save antibiotics for future illnesses.
- Never take antibiotics prescribed to someone else.
- Talk to your doctor about recommended vaccines for you and your family to prevent illnesses that require antibiotics.
- Never pressure your doctor to prescribe an antibiotic.
Healthy Bacteria
Not all bacteria is bad for you. Remember that your body has friendly bacteria that helps keep it healthy. Overuse of antibiotics can not only lead to antibiotic resistance but can harm the healthy bacteria. Loss of healthy bacteria can put you at risk of developing “opportunistic” infections when bacteria from the environment gets into the body and overruns friendly bacteria. In other cases, opportunistic infections start from a disturbance in your body due to antibiotics, which causes friendly bacteria to multiply too quickly and become harmful. Your risk of harming friendly bacteria increases if you take antibiotics too often or over long periods of time.