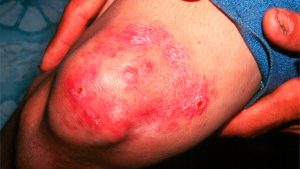
What is Plantar Fasciitis?
Plantar fasciitis is the most common cause of heel pain and affects 10 per cent of the population. The foot has a fibrous band, called fascia, which connects the heel bone to the base of the toes. When this band becomes inflamed it can result in pain and make walking difficult. Plantar fasciitis affects both men and women, but more so women and has little to do with genetics other than in having flat feet, high arches or a tight achilles tendon. Causes are mainly related to lifestyle choices such as:
- Excessive exercise, especially long-distance running, or on downhill and uneven surfaces.
- Sudden weight gain, obesity.
- Wearing shoes with poor arch support.
- Wearing shoes that don’t fit or are worn out.
- Sudden change in physical activities.
- Working in jobs with prolonged standing.
- Slow damage (micro-tears) over many months to tissue.
By the Numbers
- An estimated 1 one in 10 people will develop plantar fasciitis in their lifetime.
- 70 per cent of plantar fasciitis patients are obese.
- Plantar fasciitis patients account for between 11 per cent and 15 per cent of people who seek professional care for chronic heel pain.
Do you have Plantar Fasciitis?
Many people experience cramping or pain after working out, but how do you know if it’s something more serious? If you have been experiencing heel pain for a period of weeks a podiatrist. The pain associated with plantar fasciitis flares up more commonly:
- In the morning.
- After extended standing.
- After working out.
- While walking or running.
- While climbing stairs.
In addition to looking at your feet, your doctor will discuss daily physical activities, past injuries and past bouts of foot pain. If the pain isn’t plantar fasciitis, it could be linked to severe conditions such as bone infection or nerve damage, symptoms of which include:
- Numbness or tingling sensations in the feet.
- The foot feeling abnormally hot; has a temperature of 100.4F or above.
- The heel is swollen or stiff.
Tests
Your doctor may take an x-ray, but a physical exam will look for swelling, redness, tightness on the arch of the foot, and pain in the heel and sole. Surgery is the last line of treatment, are valuable:
- Lateral radiograph: The first level of imaging, lateral radiographs can measure the heel spur, thickness of plantar fascia and quality of the fat pad.
- Ultrasound examination: This test, used if a diagnosis is unclear, this test measures the thickness of plantar fascia, which usually ranges from 2mm-3mm in the ultrasound, but then thickens to 4mm from collected fluid.
- Plantar fascia thickness values: This is a measurement used to assess effectiveness of treatment, judged by decreased thickness in plantar fascia.
- MRI scan: Used in rare cases, when another cause of heel pain is suspected. If pain management fails, an MRI can be used to look for soft tissue, bone tumors, osteomyelitis, subtler arthritis or tarsal tunnel syndrome.
Treatment
If treated quickly plantar fasciitis will not become a chronic condition. Treatments are mainly non-invasive and require lifestyle changes to rest your heel. Surgery (plantar fascia release) to remove diseased tissue is a last treatment resort. The American Orthopedic Foot & Ankle Society recommends the following treatments:
- Rest the foot and keep weight off of it.
- Apply ice to the sore area for 20 minutes several times a day.
- Ask your doctor for a non-inflammatory medication.
- Stretching: This applies to both the achilles tendon and the calf area. Several specialists recommend calf stretching.
- Orthotics (boots, braces or splints): An example of one of these is a night splint. This supportive splint stretches the calf and the plantar fascia during the night.
- Local steroid injections: Studies have proven a significant reduction in thickness of plantar fascia as early as two weeks following a steroid injection.
All feet are unique, so talk to your doctor if you think you have plantar fasciitis.
Be Kind to your Feet
It’s all about moderation.
- Exercise moderately to prevent weight gain.
- Wear he right size shoe. Your feet change shape, whether from ageing or even pregnancy. Get your feet measured by a professional to determine the correct shoe size.
- Run on good, even terrain.
- Shoes should be replaced regularly. Experts recommend sports shoes are replaced after you’ve covered about 500 miles in them.
- Avoid walking barefoot on hard ground.
- Wear supportive footwear. Avoid wearing heels. Ideal shoes have laces and a low to moderate heel.
- Balance between sitting and standing throughout the day.